 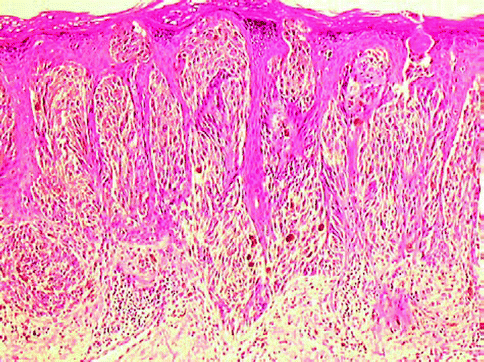
4ĭifferential diagnosis for choroidal melanoma should include choroidal hemangioma, choroidal metastases, choroidal osteoma, choroidal neurofibroma, peripheral melanocytoma, benign lymphoid tumor, extramacular disciform lesion, posterior scleritis, localized choroidal detachment with hemorrhage, congenital hypertrophy of retinal pigment epithelium (RPE) cells, RPE hyperplasia, RPE window defect, hemorrhagic retinal detachment, retinoschisis with hemorrhage, intraocular foreign body, granuloma, acquired retinal hemangioma, and traumatic angle recession. Fine-needle biopsy may be used transsclerally to confirm the presence of a malignancy. 3 It is not uncommon to order this entire battery of tests as soon as a suspicious lesion is detected. If any of these are abnormal, further testing, such as liver ultrasound, and PET/CT scan or MRI of the chest and abdomen, is required. Initial testing for metastases includes liver panels, CBC with differential, and chest x-ray. 1-3 Extrapolating from known incidence of ocular tumors, a ciliary body–based melanoma has a US incidence of about one in 1 million persons per year. Choroidal melanomas represent 85% of uveal melanomas, 10% are ciliary body, and 5% iris tissue. The uveal tissue of the eye consists of three structures: iris, choroid, and ciliary body. Within 13 days of the initial appointment, the pathology department had completed its assessment of the specimen and other testing. The timeline of this case from the first appointment to enucleation was 7 days: initial detection, diagnosis, referral to a retinal physician who specializes in ocular oncology, consultation, oncology workup, and enucleation. Cross-section of the patient’s enucleated eye showing proliferation of the ciliary body–based melanoma, displacement of the posterior chamber IOL, and associated retinal detachment. Light microscopy also revealed invasion of the iris root, trabecular meshwork, melanocytes, and macrophages in the trabecular meshwork opposite the primary tumor site.įigure 4. A central cavitation indicated that necrotic changes were starting. The tumor did not break through the sclera. Spindle-shaped melanocytes comprised the majority of the tumor, with rare epithelioid cells. Histologic analysis was performed on the enucleated eye (Figure 4). Complete blood count (CBC) and differential, comprehensive metabolic panel, and lactate dehydrogenase were all within normal ranges. No evidence of metastatic disease was found within the chest, intrapelvic or intraabdominal areas on CT imaging. The patient was scheduled for enucleation and additional workup for metastases. The mass was further classified as an iridociliochoroidal melanoma after fine needle biopsy. The patient was diagnosed with a ciliary body–based melanoma and referred urgently to retinal oncology. B-scan ultrasound of the patient’s left eye showing the 10.2-mm length of the tumor. Gonioscopy revealed an atypical superior temporal angle with a large brown mass between the iris and the choroid 0.5 mm nasally (Figure 2).įigure 3. Further examination of the iris root suggested strongly that the ciliary body had proliferated enough to displace the iris at the root and the ciliary body proliferations had begun to fill the angle. It was apparent that the iris root was pulled away from its normal limbal insertion (Figure 1). Anterior segment examination revealed sectoral injection of the superior to superotemporal conjunctival vessels of the left eye. She noticed that her left eye had also become slightly more light-sensitive, accompanied by a mild dull ache from inside her eye.īCVA was 20/25+2 OD and 20/400 OS. Efficient, integrated medical care is essential in caring for patients with choroidal melanoma.Īn 81-year-old White woman reported to our office with a complaint of vision worsening in her left eye for a duration of 2 months.Diagnosis of choroidal melanoma can be facilitated by B-scan ultrasound, blood work, fine-needle biopsy, and other imaging techniques.Intraocular melanomas are rare in everyday practice, but it is important to understand their incidence, origin, morphology, treatment methods, and overall outcomes. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
